Diseases and Conditions › Sleep Disorders › Sleep Disorders: Types, Diagnosis, Risk Factors, and Prevention
Getting a good night's sleep is essential for feeling refreshed and alert during the day. Unfortunately, not everyone is able to get the restorative sleep they need.
According to the National Institute of Neurological Disorders and Stroke, chronic, long-term sleep disorders affect at least 40 million Americans each year. Left untreated, sleep disorders, and the resulting sleep deprivation, will likely interfere with your work, driving, and social activities and have negative effects on your physical and mental well-being.
What is a sleep disorder?
The National Institutes of Health define a sleep disorder as any difficulties related to sleeping, including:
* difficulty falling or staying asleep,
* falling asleep at inappropriate times,
* excessive total sleep time, or
* abnormal behaviors associated with sleep.
Physicians and sleep specialists typically categorize sleep disorders into four main categories specified by the International Classification of Sleep Disorders. These include:
* dyssomnias,
* parasomnias,
* medical/psychiatric disorders, and
* proposed sleep disorders.
Dyssomnias
Dyssomnias are disturbances in the amount, timing, or quality of sleep resulting in excessive daytime sleepiness or insomnia. The International Classification of Sleep Disorders lists three subcategories of dyssomnias:
1) Intrinsic sleep disorders originate inside the body and are due to a variety of possible causes. Common intrinsic sleep disorders include: psychophysiologic insomnia, idiopathic insomnia, narcolepsy, obstructive sleep apnea, central sleep apnea, restless legs syndrome, and periodic limb movements in sleep.
2) Extrinsic sleep disorders originate outside the body and are due most commonly to behavioral or environmental factors. Common extrinsic sleep disorders include:inadequate sleep hygiene, environmental sleep disorder, insufficient sleep syndrome, stimulant-dependent sleep disorder, alcohol-dependent sleep disorder, and hypnotic-dependent sleep disorder.
3) Circadian rhythm sleep disorders describe the disruption of the sleep cycle in a 24-hour period. Common circadian rhythm sleep disorders include: jet lag, shift-work sleep disorder, irregular sleep-wake pattern, delayed sleep phase syndrome, and advanced sleep phase syndrome.
Parasomnias
Parasomnias are disorders of partial arousal or disorders that interfere with sleep stage transitions. Abnormal events occur during sleep. The International Classification of Sleep Disorders lists four subcategories of dyssomnias:
1) Arousal disorders are disorders of partial arousal. Common arousal disorders include: confusional arousals, sleepwalking, and sleep terrors.
2) Sleep-wake transition disorders are disorders that interfere with sleep stage transitions. Common examples include: rhythmic movement disorder, sleep starts, sleeptalking, and nocturnal leg cramps.
4) Other parasomnias include common sleep disorders such as sleep bruxism (teeth grinding), sleep enuresis (bedwetting), primary snoring, infant sleep apnea, and sudden infant death syndrome (SIDS).
Parasomnias usually associated with rapid eye movement (REM) sleep occur during the REM sleep stage. Common examples include: nightmares, sleep paralysis, and REM sleep behavior disorder
Medical/psychiatric sleep disorders
1) Sleep disorders are often attributed to medical or psychiatric disorders. The International Classification of Sleep Disorders lists three subcategories of medical/psychiatric sleep disorders:
2) Sleep disorders associated with medical disorders. Common examples include: alcoholism, chronic obstructive pulmonary disease, asthma, sleep-related gastroesophageal reflux, peptic ulcer, and fibrositis syndrome.
Sleep disorders associated with neurological disorders. Common examples include: degenerative brain disorders, dementia, sleep-related epilepsy, and sleep-related headaches.
3) Sleep disorders associated with psychiatric disorders. Psychoses, anxiety, depression, and panic disorders can result in excessive sleepiness, insomnia, or other disruptions in the sleep cycle.
Proposed sleep disorders
Proposed sleep disorders encompass sleep problems for which there is not enough information available to positively establish them as distinct disorders. Examples in this category include:
1) short sleepers (someone who regularly sleeps less than 75% of the sleep time typically required for his or her age group but feels no negative effects from this shortened sleep),
2) long sleepers (someone who regularly sleeps more than 10 hours a night),
3) subwakefulness syndrome (lack of daytime alertness with no apparent sleep disruption),
4) fragmentary myoclonus (brief, involuntary jerks or twitches), sleep hyperhydrosis (night sweats),
5) menstrual-associated sleep disorder,
6) pregnancy-associated sleep disorder,
7) terrifying hypnagogic hallucinations,
8) sleep-related laryngospasm, and
9) sleep choking syndrome.
What are the most common types of sleep disorders?
It is estimated that there are over 100 types of sleep disorders. Common sleep disorders are outlined below.
1) Sleep apnea
Sleep apnea is a breathing problem during sleep that creates a sleep disorder. Sleep apnea occurs when a person's breathing is interrupted during sleep. Distinctive signs of sleep apnea include:
- frequent waking episodes at night
- disrupted breathing, gasping, gagging, or choking for air during sleep
There are three types of sleep apnea:
- Obstructive sleep apnea (OSA): Obstructive sleep apnea is the most common type of sleep apnea and is caused by an obstruction in the airway, which actually stops the air flow in the nose and mouth. Throat and abdominal breathing continue normally. Obstructive sleep apnea is commonly accompanied by snoring and causes the sleeper to wake up, gasping or snorting, and then go back to sleep again.
- Central sleep apnea (
* irregular heartbeat,
* high blood pressure,
* heart attack, and/or
* stroke.
- Mixed sleep apnea: If you experience a combination of Obstructive sleep apnea and Central sleep apnea, you have mixed sleep apnea. Mixed sleep apnea is most commonly found in infants or young children who have abnormal breathing control.
Sleep apnea is a very serious sleep disorder. A doctor or sleep center can help assess your condition and recommend appropriate treatment. See Helpguide’s Sleep Apnea: Symptoms, Causes, Diagnosis, and Treatment for more information.
2) Restless legs syndrome (RLS) and periodic limb movement in sleep (PLMS)
Restless legs syndrome (RLS) is a neurological disorder characterized by uncomfortable, tingly or creeping sensations in your legs, which create an uncontrollable urge to keep them moving.
Symptoms of RLS include:
- irritating sensations in your legs that give you an overwhelming urge to walk around and move them
- little movements of the toes, feet or legs may be visible when you rest
- very restless sleep
Similarly, people with periodic limb movement in sleep (PLMS) experience rhythmic jerking of the feet or legs, which interrupts sleep.
While there is no cure for these disorders, treatment is highly effective – 90% of those treated experience relief of their symptoms through lifestyle changes and medication. See Helpguide's Restless Legs Syndrome (RLS) and Periodic Limb Movements in Sleep (PLMS): Symptoms, Causes, Diagnosis, and Treatment for more information.
3) Narcolepsy
Narcolepsy is a chronic neurological disorder that impairs the ability of the central nervous system to regulate sleep. People with narcolepsy experience:
- excessive daytime sleepiness and
- intermittent, uncontrollable episodes of falling asleep during the daytime.
Other symptoms typically associated with narcolepsy include:
- cataplexy (short-lived intermittent muscle weakness),
- hypnagogic hallucinations (hallucinations while falling asleep or waking),
- sleep paralysis (paralysis while falling asleep or waking), and
- automatic behavior.
Narcolepsy usually begins when a person is in their teens or early twenties. Doctors typically recommend a combination of medication and behavioral treatments for the condition. See Helpguide's Narcolepsy: Symptoms, Causes, Diagnosis and Treatment for more information.
4) Parasomnias
Parasomnias encompass a number of disruptive sleep events, or "disorders of arousal," including:
* Sleep walking and sleep talking
* Sleep terrors and nightmares
* Partial seizures
* Violent behavior during sleep
* Sleep-related eating or drinking disorders
* REM sleep behavior disorder (acting out dreams)
Often, a person does not recall their experience of the parasomnic event the following day. Parasomnias are often attributed to stress, depression, or other psychological and medical conditions. Treatment for parasomnias may involve lifestyle changes, medication, hypnosis, guided imagery, or some combination thereof. Your physician or sleep specialist can assist you in finding the best-suited treatment based on your individual symptoms. To find a sleep specialist near you, see references & resources.
Do you have a sleep disorder?
The 2005 Sleep in America Poll conducted by the National Sleep Foundation found that of the 20% of respondents who usually take more than 30 minutes to fall asleep:
* 44% think they have a sleep problem
* 82% experience at least 1 symptom of insomnia
* 44% experience daytime sleepiness at least 3 days a week
* 32% report that they get less sleep than they need to perform at their best
* 44% have problems in their relationship due to their partner’s sleep disorder
If you consistently have trouble sleeping at night, you may be one of 70 million Americans who suffer from sleep disturbances each year. Because there are over 100 types of sleep disorders, it might be difficult to figure out what is affecting your sleep. It is important to explore the possible causes of your sleeplessness and try to find a solution.
One way to evaluate the quality of your sleep is to think about how you feel during normal daytime activities. If you are experiencing one or more of the following characteristics, you may not be getting proper sleep at night (information provided by the National Institutes of Health).
Do you . . .
* fall asleep while driving?
* struggle to stay awake when inactive, such as when watching television or reading?
* have difficulty paying attention or concentrating at work, school, or home?
* have performance problems at work or school?
* often get told by others that you look sleepy?
* have difficulty remembering?
* have slowed responses?
* have difficulty controlling your emotions?
* need to take naps almost every day?
How are sleep disorders diagnosed?
Sleep disorders are often diagnosed based on a number of factors including your
* description of symptoms
* age and gender
* psychological history
* medical history
* family member or partner’s observation of disruptive sleep patterns
In order to determine if you have a sleep disorder, it is important to pay attention to your sleep habits and daily routine. Keeping a sleep diary (see Helpguide’s sample sleep diary) may be helpful in discussing your daily patterns with your doctor or sleep specialist.
Other methods physicians and sleep specialists use to diagnose sleep disorders include:
1) Epworth Sleepiness Scale – This sleep questionnaire asks you to rank whether certain situations make you sleepy and, if so, how sleepy. Your responses will assist your doctor in providing a formal diagnosis.
2) Nocturnal polysomnogram - This test will measure the electrical activity of your brain (electroencephalogram) and heart (electrocardiogram), and the movement of your muscles (electromyogram) and eyes (electro-oculogram) and usually requires an overnight stay at a sleep clinic for observation purposes.
3) Multiple sleep latency test (MSLT) – This test measures how long it takes for you to fall asleep during the day. Sleep specialists will observe your sleep patterns.
4) Repeated test of sustained wakefulness (RTSW) –This test measures how long it takes for you to fall asleep by challenging your ability to stay awake. During the test, you will likely be placed in a quiet room with dim lighting and asked to stay awake.
5) Blood test – Depending on your description of your symptoms and personal and family medical histories, a blood test may also be conducted. The blood test may not be conclusive but can be helpful in establishing the possibility and probability of certain sleep disorders.
While most common sleep problems can be addressed through making lifestyle changes and developing an improved sleep hygiene routine (see Helpguide’s Insomnia: Causes, Cures and Treatments and Tips for a Good Night's Sleep for more information), it is important to see your doctor or a sleep specialist if your sleep does not improve. To find a sleep specialist near you, see references & resources.
Are you at risk of developing a sleep disorder?
There are many things you can do to reduce your risk of developing a sleep disorder. By making small changes, you can greatly improve the quality of your sleep and thereby the overall quality of your mental and physical well-being. If you find that you currently practice or experience one or more of the following risk factors, you may want to consider making changes to your lifestyle or consulting with your doctor to learn how you can improve your health:
* poor sleep environment (i.e., noisy or brightly lit)
* excessive caffeine or alcohol intake
* use of certain medications and drugs
* smoking or chewing tobacco
* anxiety, depression, or other mood disorder
* stressful situation such as death of a loved one or job pressure
* counter-productive sleep routine
* daytime napping
* early or late-night bed times
* traveling between time zones
* shift workers with rotating schedules
* physical illness
* obesity
See Helpguide’s Tips for a Good Night’s Sleep for specific tips on reducing your risk of developing a sleep disorder.
Are there ways to prevent sleep disorders?
The National Commission on Sleep Disorders, headed by Dr. William C. Dement (a leading authority on sleep at
* educating yourself about the sleep cycle, stages, and common disorders
* developing a healthy sleep routine
* talking with your doctor or a sleep specialist about your sleep concerns
Article Source: http://www.helpguide.org/life/sleep_disorders.htm
Article By: Heather Larson, Gina Kemp, M.A., and Robert Segal, M.A., contributed to this article.
risk factors of sleep disorder
,Sleep disorders are appropriately diagnosed based on the
, sleep choking syndrome, subwakefulness syndrome, subwakefullness syndrome, restless leg syndrome, , ,describe three sleeping disorders and their characteristics
,psychological risk factor sleep disorders
,laryngospasma dignosed at sleep clinc
,arousal or disorders that interfere with sleep stage transitions
, ,is laryngospasm in sleep a type of sleep apnea
,Causes and treatment of nocturnal enuresis
, ,what type of doctor diagnoses sleep disorders
,types of sleep disorders symptoms
,risk factors of types sleep disorder
,What are the risk factors of sleeping disorder
, , , , ,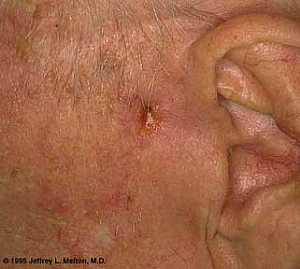 Basal Cell Carcinoma ("Rodent Ulcer" Type)
Basal Cell Carcinoma ("Rodent Ulcer" Type)
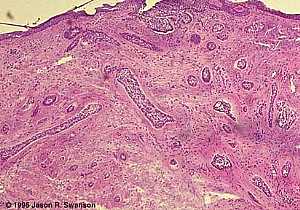 Basal Cell Carcinoma (Histology-Morpheaform Type)
Basal Cell Carcinoma (Histology-Morpheaform Type)
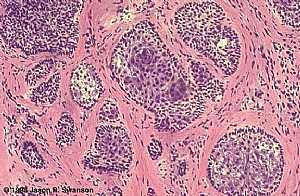 Basal Cell Carcinoma (Histology-Nodular Type - High power)
Basal Cell Carcinoma (Histology-Nodular Type - High power)
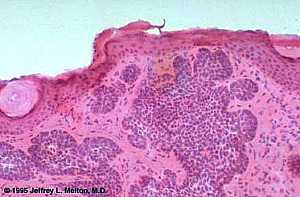 Basal Cell Carcinoma (Histology-Nodular Type- High power)
Basal Cell Carcinoma (Histology-Nodular Type- High power)
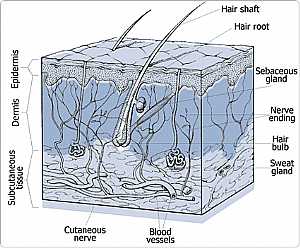 Skin
Skin
 Nervous System -- Basic
Nervous System -- Basic
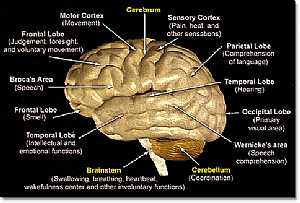 Brain anatomy
Brain anatomy
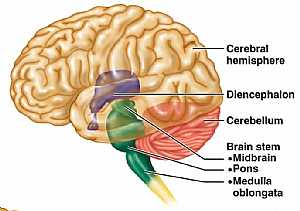 Brain anatomy
Brain anatomy
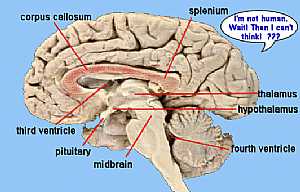 Brain anatomy
Brain anatomy
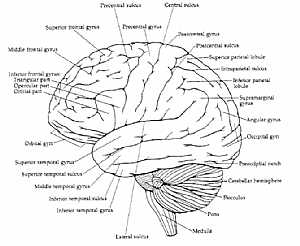 Brain anatomy
Brain anatomy
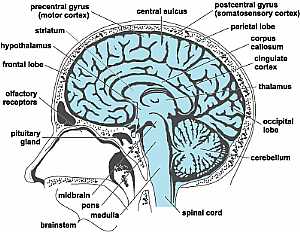 Head anatomy
Head anatomy
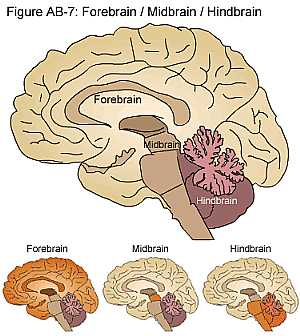 Brain anatomy
Brain anatomy
© Copyright 2001-2022 eDoctorOnline.com

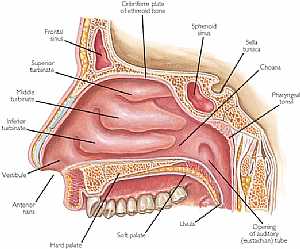 Nose anatomy
Nose anatomy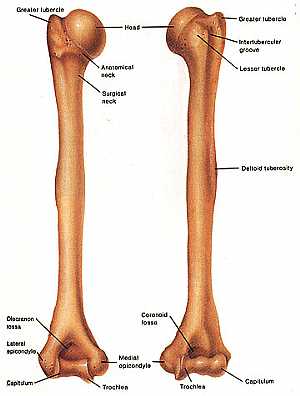 Humerus bone
Humerus bone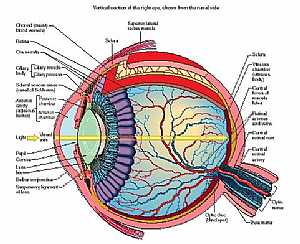 Eye anatomy
Eye anatomy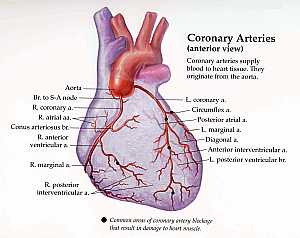 Coronary arteries anatomy
Coronary arteries anatomy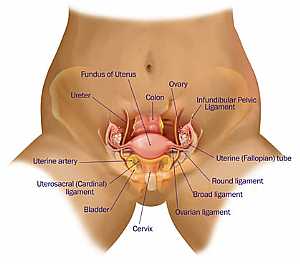 Female pelvic anatomy
Female pelvic anatomy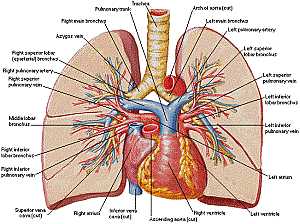 Heart and lung anatomy
Heart and lung anatomy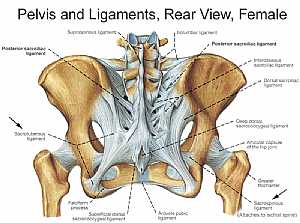 Bones and ligaments of the FEMALE Pelvis
Bones and ligaments of the FEMALE Pelvis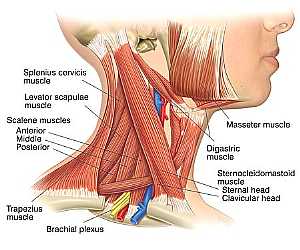 Neck Anatomy
Neck Anatomy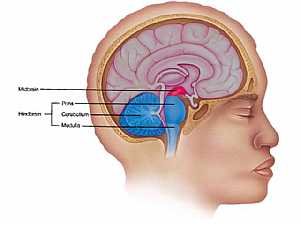 MidBrain anatomy
MidBrain anatomy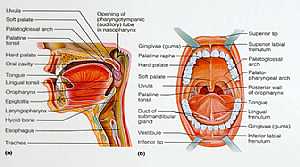 Oral Cavity
Oral Cavity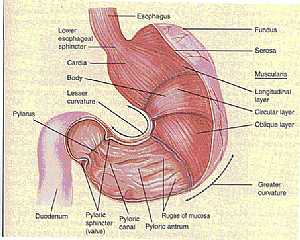 Stomach anatomy
Stomach anatomy Lung anatomy
Lung anatomy Basal Cell Carcinoma ("Rodent Ulcer" Type)
Basal Cell Carcinoma ("Rodent Ulcer" Type) Basal Cell Carcinoma (Histology-Morpheaform Type)
Basal Cell Carcinoma (Histology-Morpheaform Type) Basal Cell Carcinoma (Histology-Nodular Type - High power)
Basal Cell Carcinoma (Histology-Nodular Type - High power) Basal Cell Carcinoma (Histology-Nodular Type- High power)
Basal Cell Carcinoma (Histology-Nodular Type- High power) Skin
Skin Nervous System -- Basic
Nervous System -- Basic Brain anatomy
Brain anatomy Brain anatomy
Brain anatomy Brain anatomy
Brain anatomy Brain anatomy
Brain anatomy Head anatomy
Head anatomy Brain anatomy
Brain anatomy
Be the first one to comment on this article!