Articles for Physicians - Articles by Doctors › Case Reports › Miller Fisher Syndrome: A Case Report
Introduction:
Miller Fisher Syndrome is a rare variant of Guillain-Barre syndrome resulting in a post-infectious neuropathy that affects 0.1 per 100,000 worldwide annually. Miller Fisher syndrome presents with a triad of areflexia, ataxia and ophthalmoplegia. This typical presentation of Miller Fischer syndrome is not always evident. In this paper, we introduce a case of a young female who presented during the summertime with the triad stated above plus facial and transient lower limb parasthesia.
Case Report:
A previously healthy, 40 year old Latin American female presented with a 10 day history of slurred speech and unsteady gait. Days prior to onset of symptoms, the patient suffered from 24 hour gastroenteritis with multiple episodes of diarrhea. The patient attempted to receive care at another facility for the neurological symptoms but left due to frustration at the lack of diagnosis and treatment. Upon presentation, the patient was anxious, afebrile, with horizontal diplopia in the right eye and ataxia gait. Her past medical history, family and social histories were unremarkable. Patient denied any travel history, recent insect or animal contact.
Cranial nerve examination revealed opthalmoplegia with loss of abduction of the right eye. Pupillary reflexes and light accommodation were both intact. She had bilateral facial palsy resulting in dysarthria without aphasia. Facial sensory deficits were noted bilaterally in the right the trigeminal nerve distribution.Examination of the patient’s peripheral nervous system revealed moderate loss of muscle strength upon thigh extension more prominent in the right lower extremity than the left.The upper extremities displayed equal muscle strength.Vibratory sensation was intact.On testing of proprioception patient showed increased body postural swaying with eyes closed.The patellar reflex on both left and right were moderately diminished.
Leukocyte count on admission was within normal limits and remained relatively constant throughout her hospital course.The patient’s electrolytes, B12, and ESR were within normal limits. Both MRI with contrast, carotid ultrasound, and CT without contrast showed no abnormalities. CT of the abdomen and chest revealed left axillary lymphadenopathy. Nerve conduction studies showed normal motor conduction velocity with reduction of sensory nerve responses.
A lumbar puncture performed on the second day showed clear cerebral spinal fluid (CSF), WBC 9, RBC 13, elevated Protein concentration of 119mg/dl, Glucose 54mg/dl, with 100 lymphocytes. CSF serology showed nonreactive VDRL, no detection of West Nile antibodies, or bacterial antigen for streptococcus, meningococcus, haemophilis and cryptococcus. Serum Lyme titers were unremarkable and patient’s HIV status was negative.
On second day of admission, the patient was placed on intravenous immunoglobin at a dose of 0.4g/kg/day. The patient experienced no side effects from treatment.After ninety six hours of treatment the patient began to show improvement in her symptoms and was able to move around the hospital room with assistance. The patient was discharged four days after initiation of the intravenous immunoglobulin and in total received 1.6g/kg/day. Patient asked to follow up at the neurology clinic and breast clinic for the lymphadenopathy. The patient’s symptoms completely resolved five weeks later.
Discussion:
Miller Fisher Syndrome is a rare variant of Guillain-Barre syndrome that presents after a viral infection. Miller Fisher is one of the only Guillain-Barre variants that does not present with generalized weakness. This syndrome manifests as a descending paralysis with a triad of opthalmoplegia, ataxia and areflexia. It is considered a benign cause of acute demylelinating polyneuropathy that resolves in a matter of weeks. Even though this syndrome has a benign course for the patient these symptoms can be alarming.
In Miller Fisher syndrome, the male to female ratio is 2:1 with a mean age of 43yrs. Viral infections precede onset of syndrome by about 10 days before neurological deficits appear. The external ophthalmoplegia usually presents first and begins symmetrically with loss of abduction. Approximately half of the cases do not have typical presentation but have additional signs of neuropathy such as facial weakness or oropharyngeal weakness. About 10% will initially have some proximal muscle weakness that can progress to Guillian-Barre.
Miller Fisher is highly associated with Campylobacter jejuni enteritis (7). Post-infectious syndromes result from an auto-immune attack on gangliosides which are an important neuronal membrane component. An example of post-infectious auto-immunity is antibodies attacking host gangliosides secondary to molecular mimicry between host gangliosides and Campylobacter jejuni lipopolysacharides (7). Many studies have shown that Anti GQ1b (a ganglioside nerve component) IgG antibodies are found 90% of the time in the patient’s serum. This antibody is part of syndrome pathogenesis and occurrence of opthalmoplegia. GQ1b gangliosides are found in the 2nd, 3rd, 4th and 6th cranial nerves. These antibodies are increased during the syndrome, than decrease with resolution of symptoms and are eventually undetectable in 2 years (8). Miller Fisher syndrome affects peripheral nerves like Guillian Barre with both syndromes having similar pathology (4).
Treatment consists of intravenous immunoglobulin, which is very expensive and can have severe side effects. Minor complications with IV immunoglobulins occur 59% of the time and approximately 5% can have serious complications including congestive heart failure, renal failure and cerebral infarction. This treatment has been shown to decrease severity and length of disease (5).
Diagnosis of Miller Fisher can be made based on patients post infectious history, triad presentation (ataxia, areflexia, ophthalmoplegia. CSF fluid analysis with elevated protein, normal WBC count, nerve conduction abnormalities and serum antibodies directed against nerve components (1). Other differentials should be considered and explored such as Lyme disease, Multiple sclerosis, HIV, B12 deficiency, 3rd stage syphilis, West Nile virus, Myasthenia gravis, Sarcoidosis and stroke.
The prognosis for Miller Fisher syndrome is good with a mean recovery time for patients of approximately 10 weeks. Patients diagnosed with Miller Fisher can have multiple reoccurrences with later viral infections (2).
References:
1.Clinical features and Diagnosis of Guillain-Barre Syndrome in Adults, www.uptodate.com
2.Dewarrat A, Regli F, Steck A et al: Recurrent Miller Fisher Syndrome. Significance of anti GQ1b antibodies.Schweiz Arch Neurol Psychiatry 1995; 146:180-184
3.Fisher M: An unusual Variant of Acute Idiopathic polyneuritis (syndrome of ophthalmoplegia, ataxia and areflexia. New England Journal of Med 1956; 255: 57-65
4.Hughes Richard AC, Cornblath David R: Guillain-Barre Syndrome. Lancet 2005; 366:1653-63
5.Mori M, Kuwabara S, Fukutake T, Hattori T: Intravenous immunoglobulin therapy for Miller Fisher syndrome. Neurology 2007; 68:1144-1146
6.Phillips MS, Stewart S, Anderson JR: Neuropathological findings in Miller Fisher Syndrome. Journal Neurosurg Psychiatry 1984; 47:492
7.Salloway S, Mermel LA, Seamans M, Aspinall GO, et al: Miller Fisher Syndrome associated with Campylobacter jejuni bearing Lipopolysacharide molecules that mimic Human Ganglioside GD3. Infection and Immunity 1996; 2945-2949
8.Yuan Chih-Lun, Wang Yuh Jen, Tsai Ching Piao: Miller Fisher Syndrome: A Hospital based Retrospective study. European Neurology 2000; 44:79-85
9.Yuki N, Taki T, Takahashi M, et al: Molecular mimicry between GQ1b Ganglioside and Liposacharides of Campylobacter jejuni isolated from patients with Fishers syndrome. Ann Neurol 1994; 95-106
Article By: Tiffany A. Pompa
Causes and Treatment of Stress
Haiti - Medical Cataclysm
Portal Venous System Thrombosis Following Splenectomy
A Case of Abruptio Placentae with a History of H1N1 Influenza Infection
An interesting case of Hypokalemic periodic paralysis
Fracture of malleus and dislocation of multiple ossicular joints after welding flame burn
Erythema induratum: a case of mistaken identity
Fracture of malleus and dislocation of multiple ossicular joints after welding flame burn
A liver fibrosis cocktail? Psoriasis, methotrexate and genetic hemochromatosis
Acute unilateral hearing loss as an unusual presentation of cholesteatoma
An interesting case of Hypokalemic periodic paralysis
A Case of Abruptio Placentae with a History of H1N1 Influenza Infection
Bilateral neuro-retinitis following chick embryo cell anti-rabies vaccination – a case report
Portal Venous System Thrombosis Following Splenectomy
miller fisher syndrome
,mss
, MILLER FISHER, Miller Fisher Virus, miller fisher case report, miller fisher syndrome case reports, ,miller fisher syndrome uptodate
, ,miller fisher syndrome recovery time
,miller fisher syndrome case report
, , ,how many cases of miller fisher syndrome
,miller fisher syndrome symptoms
, , ,csf findings in miller fisher syndrome
,miller fisher syndrome a case study
,recovery time from miller fisher syndrome
,miller fisher syndrome with hearing impairment
, ,b12 deficiency and miller fisher syndrome
, ,introduction miller fisher syndrome
, ,case series on miller fischer varient
,wordwide study about miller fisher symdrome
, , ,hunter fisher syndrome with facial paralysis
,lumbar puncture miller fisher syndrome
,csf study for miller fisher uptodate
,miller fisher syndrome case study
,fisher and stewart carse report
,how does one get miller fischer variant of guillain barre syndrome
,miller fischer syndrome complications
,miller fisher with postural drop
, ,miller fisher syndrome and vit b12
, ,miller fisher and horizontal diplopia
,how does one get infected with miller fisher syndrome
, ,miller fisher variante disease diagnosis
,miller fisher syndrome and pregnancy
,algorithm in diagnosis of miller fisher
, , , ,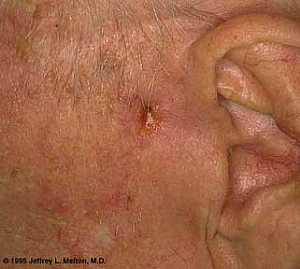 Basal Cell Carcinoma ("Rodent Ulcer" Type)
Basal Cell Carcinoma ("Rodent Ulcer" Type)
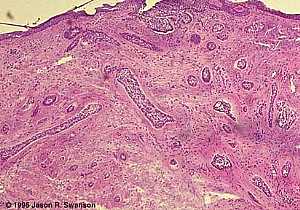 Basal Cell Carcinoma (Histology-Morpheaform Type)
Basal Cell Carcinoma (Histology-Morpheaform Type)
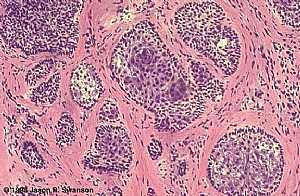 Basal Cell Carcinoma (Histology-Nodular Type - High power)
Basal Cell Carcinoma (Histology-Nodular Type - High power)
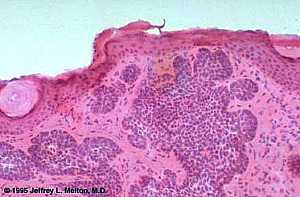 Basal Cell Carcinoma (Histology-Nodular Type- High power)
Basal Cell Carcinoma (Histology-Nodular Type- High power)
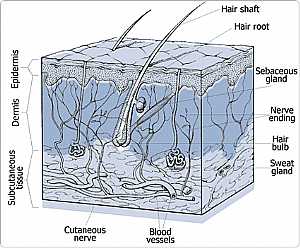 Skin
Skin
 Nervous System -- Basic
Nervous System -- Basic
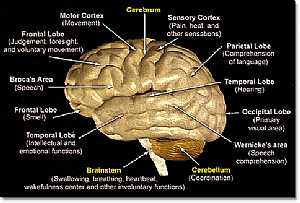 Brain anatomy
Brain anatomy
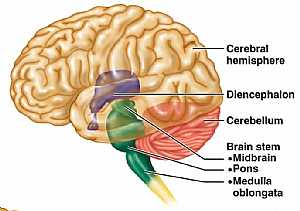 Brain anatomy
Brain anatomy
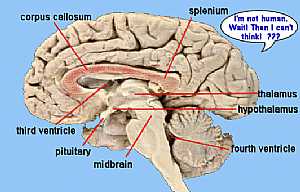 Brain anatomy
Brain anatomy
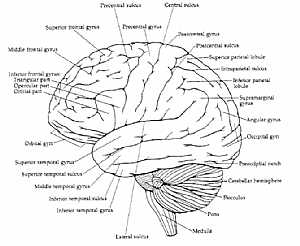 Brain anatomy
Brain anatomy
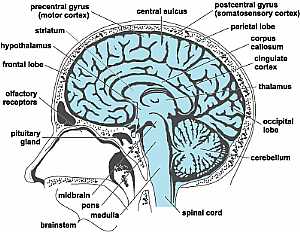 Head anatomy
Head anatomy
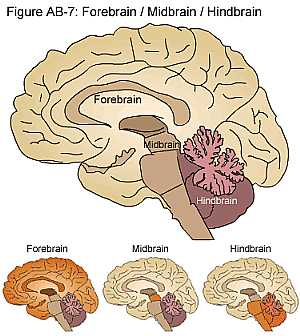 Brain anatomy
Brain anatomy
© Copyright 2001-2022 eDoctorOnline.com

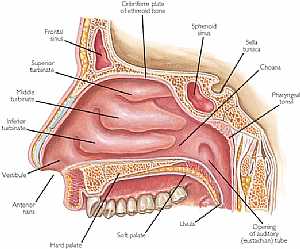 Nose anatomy
Nose anatomy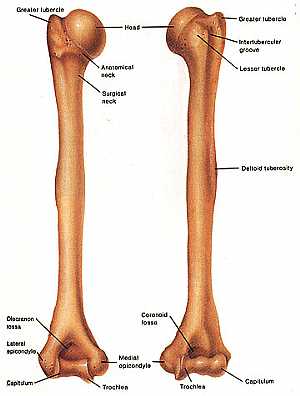 Humerus bone
Humerus bone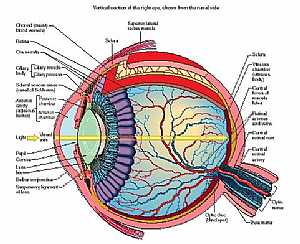 Eye anatomy
Eye anatomy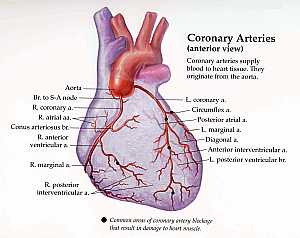 Coronary arteries anatomy
Coronary arteries anatomy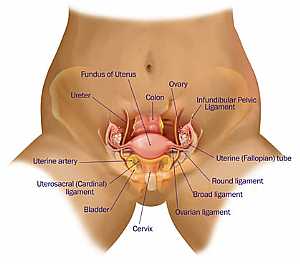 Female pelvic anatomy
Female pelvic anatomy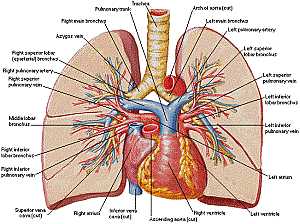 Heart and lung anatomy
Heart and lung anatomy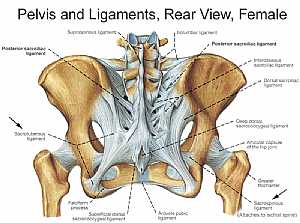 Bones and ligaments of the FEMALE Pelvis
Bones and ligaments of the FEMALE Pelvis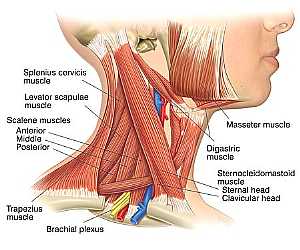 Neck Anatomy
Neck Anatomy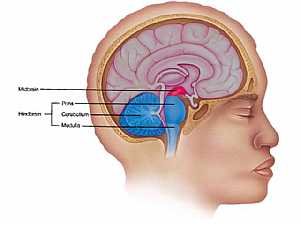 MidBrain anatomy
MidBrain anatomy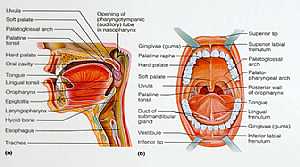 Oral Cavity
Oral Cavity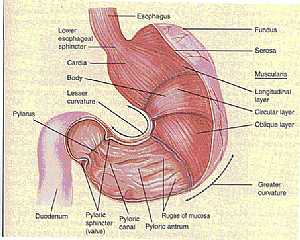 Stomach anatomy
Stomach anatomy Lung anatomy
Lung anatomy Basal Cell Carcinoma ("Rodent Ulcer" Type)
Basal Cell Carcinoma ("Rodent Ulcer" Type) Basal Cell Carcinoma (Histology-Morpheaform Type)
Basal Cell Carcinoma (Histology-Morpheaform Type) Basal Cell Carcinoma (Histology-Nodular Type - High power)
Basal Cell Carcinoma (Histology-Nodular Type - High power) Basal Cell Carcinoma (Histology-Nodular Type- High power)
Basal Cell Carcinoma (Histology-Nodular Type- High power) Skin
Skin Nervous System -- Basic
Nervous System -- Basic Brain anatomy
Brain anatomy Brain anatomy
Brain anatomy Brain anatomy
Brain anatomy Brain anatomy
Brain anatomy Head anatomy
Head anatomy Brain anatomy
Brain anatomy
I disagree with the recovery time. How have Miller Fisher for four years this October. Spent 5 months inpatient rehab and 13 months as out patient rehab. My muscles stay very tight (like they will snap), this affect my gait (been told I shouldn't be able to walk) but I can walk without support for one mile. My eating, speech, writing, etc. I had to learn everything over (I mean everything). Numbness throughout the body. Haven't gave up hope yet. My question will U finally return to normal